Many of our patients come to the Bunion Institute with heads full of common myths they may have heard from friends or on social media. It’s always best to go to the experts when facing a troubling medical condition, not common myths or social media. Bunion Institute’s nationally-recognized podiatrists straighten out some common bunion misconceptions.
What is a bunion?
Also known as hallux valgus, a bunion is an irregularity on the joint at the base of the big toe. Bunions do not appear overnight; they appear gradually. That’s why it is always wise to pay us a visit at your first suspicion of a bunion.
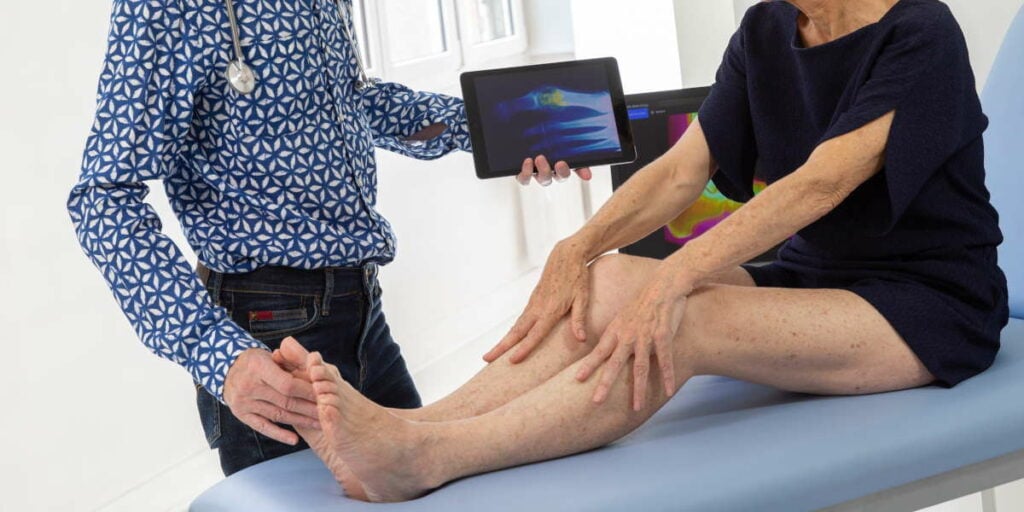
What are common bunion myths?
With the prevalence of social media, it has (unfortunately) become much easier to spread misinformation. These are six common bunion myths that need to be debunked.
Myth #1 A bunion is simply a lump of fluid
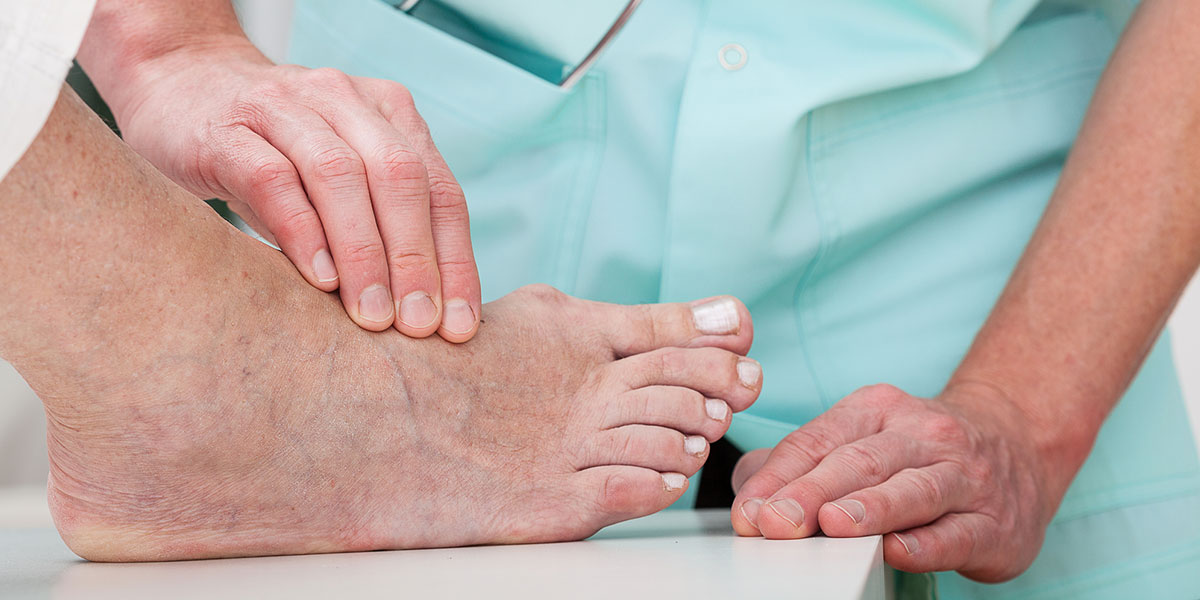
That fairy tale receives a quick no. A bunion is made of solid bone and is caused by the round surface of the 1st metatarsal sticking out. There should be a straight line between the foot and the big toe. A bunion begins to form when these two things shift out of alignment.
Here’s where the myth probably started: there may be a tiny sac of fluid that forms to take the pressure off the metatarsal prominence.
Myth #2 All bunions cause pain when walking
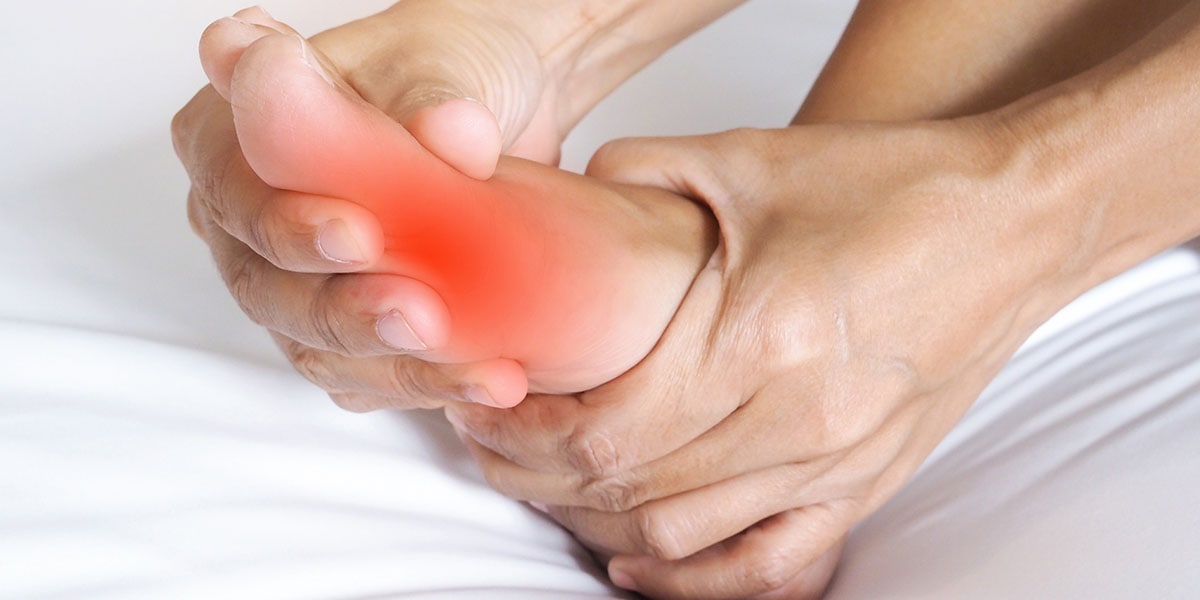
Sorry, one size bunion does not fit all. Everybody’s bunion forms differently: some manifest as small bumps with no pain; other less-fortunate people have a large lump, arch loss, chronic foot pain, and sometimes pain in the calf. It is those people who typically limp into the Bunion Institute.

Myth #3 Bunions happen because of tight shoes
Just more stories. Shoes, alone, do not cause bunions. They can be, however, major contributing factors. Bunions are caused by an instability of the big toe joint. It isn’t easy to pinpoint the exact cause of a bunion because the human foot is complicated machinery.
Most of the time, bunions have multiple causes. These include genetics, structural abnormalities, pregnancy, and tight-fitting shoes. Tight-fitting and pointed-toe shoes as well as high heels push your toes together unnaturally, so if your great toe joint is already at risk, the pressure can exacerbate your bunion formation.
Myth #4 Surgery is the only way to treat bunions
Somebody’s talking fiction. If a patient hasn’t delayed and “lived with” the bunion for too long, the Bunion Institute has excellent tools to avoid surgery. These include:
- Custom orthotics (inserts) to stabilize the foot.
- Bunion pads to reduce rubbing.
- NSAIDs (non-steroidal anti-inflammatory drugs) can be applied topically, taken orally, or injected into the bunion by your doctor to reduce pain.
- Wearing shoes with a wide toe box can reduce pain and prevent the bunion from getting worse.
- Topical compound creams may relieve pain when applied directly to the skin.
- Biofreeze sprays provide a cooling sensation to the pained area.
- Lidocaine patches numb the area for up to 12 hours.
- Steroid or cortisone may be effective but can only be used occasionally.
- Platelet-rich plasma or amniotic membrane injections can improve a painful joint.
- Range of motion exercises may soothe the foot.
Myth #5 Bunion surgery is painful
Not anymore! Surgery and recovery can be pain-free when you choose a bunion surgeon with vast experience and up-to-date bunion correction techniques. Our patients rarely need pain medications after treatment.
Post-surgical pain results from movement and swelling. Our surgeons use gentle precision with the tissue, never “hacking away.” It takes years of training and effort to perform an excellent bunion dissection.
Hypermobility in the bones is one of the leading causes of swelling and pain after surgery. Using fixation technology, the bone is appropriately held in the area of correction, resulting in less movement, less swelling of soft tissue, and less pain overall.
Our podiatrists use a proprietary long-acting local anesthesia cocktail to keep the pain away. The longer a patient is numb, the easier it is for them to get in bed, relax, and heal. Our time-tested post-surgical anti-inflammation protocols require almost no significant narcotics.
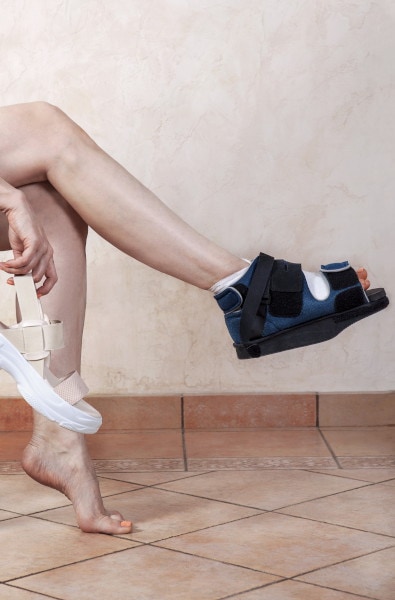
Patients exit surgery with a stability boot to immobilize the foot. Keeping the foot stable means there is less movement, less swelling, and less pain.
Myth #6 There is only one kind of bunion surgery
Nothing could be further from the truth. Over the years, at least 44 different types of bunion surgery have been performed. Our experience has allowed us to narrow down all available bunion surgeries and only perform the best procedures.
Minimally invasive bunionectomy
Minimally Invasive Bunionectomy is practiced on patients with mild to moderate bunions and good to excellent bone quality. In place of a small weak pin — which is used in most minimally invasive procedures — our proprietary technique uses stabilizing screws placed through micro-incisions. This results in quicker recovery times, reduced scarring, and less pain.
Chevron osteotomy bunionectomy
Chevron Osteotomy Bunionectomy is ideal for patients with a mild bunion and poorer bone quality or moderate bunion deformities.
For this procedure, the surgeon cuts the head of the first metatarsal, just behind the big toe joint. This chevron — or V-shaped — cut allows the surgeon to shift the first metatarsal to the second metatarsal bone. Two screws hold the bones together in their newly corrected position.
New advances in fixation technology using the OSSIOfiber® Intelligent Bone Regeneration Technology allow us to use non-metal screws that are integrated into and eventually become bone. This removes future problems from metal screws and makes your bunion correction even more secure.
This approach results in less pain, no cast, and faster recovery. It allows for immediate weight-bearing, and most patients are in regular shoes within 4 to 6 weeks. Additionally, the incision is made on the side of the foot to avoid a large visible scar on the top of the foot.
Lapiplasty® bunion correction
Lapiplasty Bunion Correction is the gold standard for patients with severe bunion deformities or compromised bone quality. The Bunion Institute perfected this surgery by adding stem cells, amniotic fluid allograft, and platelet-rich plasma.
This only procedure offers a near-zero chance of bunion recurrence for serious to severe bunion deformities. Also, lapiplasty patients have speedier recoveries, with little or no pain, less downtime, earlier weight-bearing, and minimal scarring.
Bunion surgery revision
If your first bunion surgery was unsuccessful, we offer bunion surgery revision. With this surgical process patients no longer have to suffer the poor outcomes of their previous surgery. Revision of failed bunion surgery restores motion and anatomical alignment at the great toe while improving the foot’s cosmetic appearance and relieving pain symptoms.
Bunion revision surgeries help restore motion and anatomical alignment at the great toe while improving the foot’s cosmetic appearance and relieving pain symptoms.
The prime cause for recurrence is that the wrong bunion correction procedure was performed in the first place.
Why trust the Bunion Institute with your bunion treatment?
The nationally-recognized Bunion Institute podiatry experts offer the most advanced foot care solutions and the highest foot surgery and care success rates. Our foot and ankle specialists have years of experience and are leaders in researching and treating all bunion procedures.
Serving locations throughout Southern California including Santa Monica, Sherman Oaks, Los Angeles, West Lake Village, Granada Hills, and Valencia.
Please call (855) 814-3600, or request a consultation online so that we can discuss your situation.






 Listen Now
Listen Now 



Leave a Comment